|
4/5/2024 0 Comments Abcd of medicare and medicaidCheck with your insurance plan or the study team to determine coverage. Sometimes research services are paid for by the study. Each study is different, but in many cases insurance will pay for medically necessary services that are part of the research study. The informed consent form discusses who will pay the costs of services that are part of the clinical trial. Participation in clinical research is voluntary. 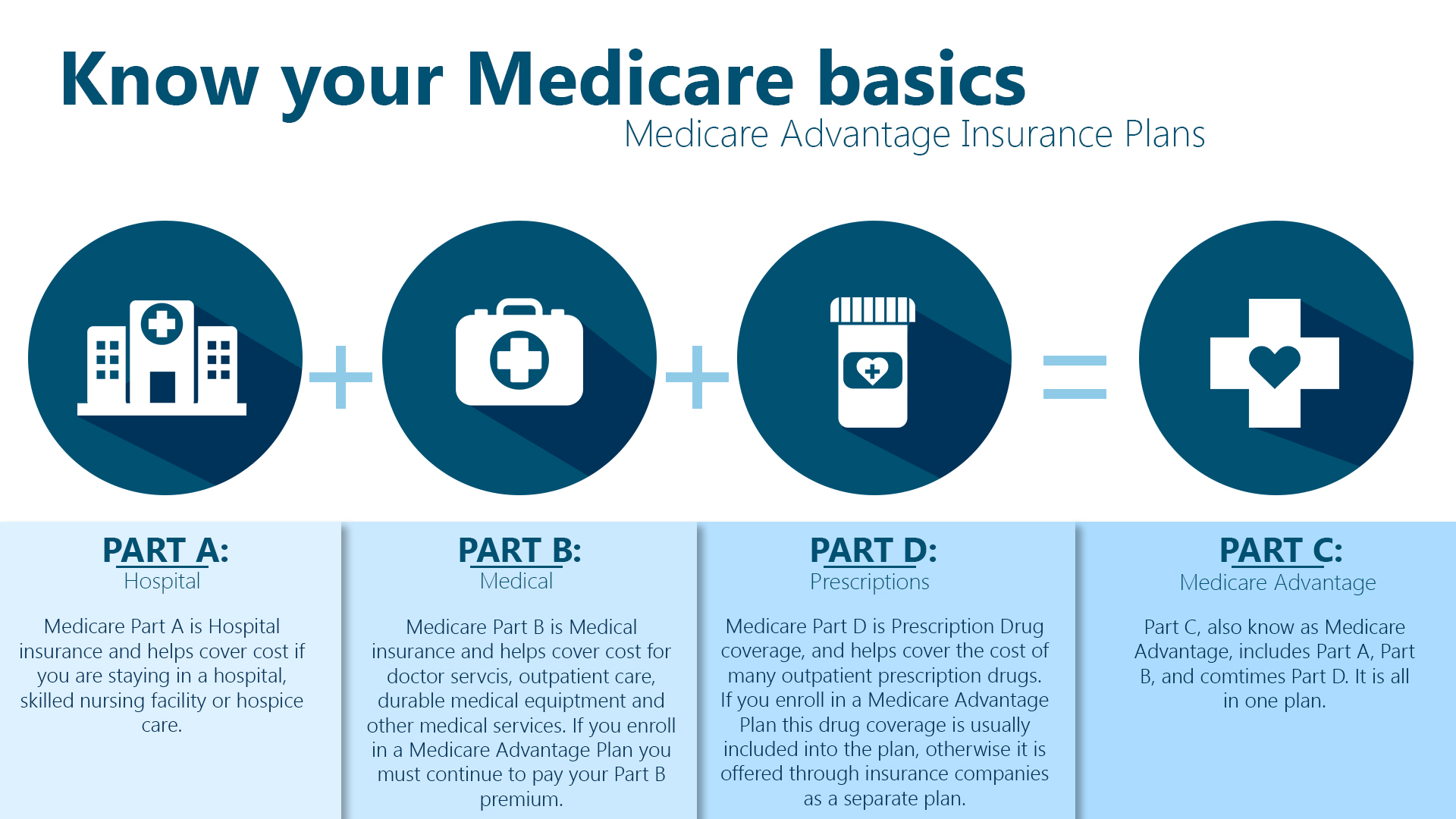
Research conducted to evaluate the safety and/or effectiveness of a treatment, diagnostic procedure, preventive measure or similar medical intervention by testing the intervention on patients in a clinical setting. In addition, CMS works with the states to run the Medicaid programs.Ĭlinical research, clinical trial or research study (Also see “Experimental or investigational treatments”) The federal agency that runs the Medicare program. Your medical bill that is sent to an insurance company for payment.Ī number assigned by your insurance company to an individual claim. ChampVA does not have a network of health care providers, so eligible members can visit most authorized providers. ChampVA shares the cost of certain medically necessary procedures and supplies with eligible beneficiaries. Also called an Authorization Number, Prior Authorization Number or Treatment Authorization Number. If you buy brand-name drugs that are not on the formulary, you often pay more because your health plan pays more.Ī number stating that your treatment has been approved by your insurance plan. This brand-name drug will cost more than the generic version, but cost less than other brand-name drugs that are not on the formulary. Your health plan formulary may list a specific brand-name drug if a price agreement has been made with that company. 
For any health need, there may be competing drugs from different companies. Brand-name drugs may or may not be listed on a formulary. Benefits may describe what portion of the allowed amount may be due from you, the level to which they will pay for services provided by various providers, and what types of services they will or will not cover.ĭrugs made and sold by a major drug company. The extent to which your insurance coverage will pay for services provided to you. A Benefits Contract is also sometimes referred to as a certificate of coverage or evidence of coverage. This contract establishes the full range of benefits available to you through your healthcare plan. The legal agreement between a health plan and you. Also called a Certification Number, Prior Authorization Number or Treatment Authorization Number.Ī way providers can retrieve information about whether you have insurance coverage. The doctor who orders your treatment and who is responsible for your care.Ī number stating that your treatment has been approved by your insurance plan. The inpatient services you receive beyond room and board charges, such as laboratory tests, therapy, surgery, etc.Ī process by which you, your doctor or your hospital, can object to your health plan when you disagree with the health plan’s decision to deny payment for your care.Ī portion of your bill, as defined by your insurance company, that you owe your provider.Īn agreement you sign that allows your insurance to pay the provider directly. What your insurance company does not pay, including deductibles, co-insurances and charges for non-covered services. Outpatient surgery or surgery that does not require an overnight hospital stay. Call your insurance company for more information. The combined total paid by you and your insurance to a provider should not exceed the allowed amount when we are in-network with your plan. This amount is usually less than the amount billed by the provider and is determined by pre-negotiated contracts or regulations. The notice is given to you so that you may decide whether to have the treatment and how to pay for it.ĭetermined by your insurance to be the amount your provider is due for a particular service. 
Words or phrases your doctor uses to describe your condition.Ī notice your provider gives you before you are treated, informing you that Medicare will not pay for the treatment or service. The portion of your bill that your provider has agreed to write off. 
The number assigned by your provider (hospital, physician, home care service, etc.) when medical services were provided.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
